North Shore – Breast Reconstruction
Dr Shagun Aggarwal is a cosmetic and reconstructive Specialist Plastic Surgeon based on the North Shore, Sydney, and at 2 prestigious public hospitals in Sydney – Prince of Wales and Royal Prince Alfred Hospitals. Dr Aggarwal is passionate about breast reconstruction and a sub-specialist in this field. In fact he pursued two international premier breast reconstruction fellowships overseas – the first at the University of Toronto, and the second in microsurgery at the University of Pennsylvania.
Currently, Dr Aggarwal performs breast reconstruction regularly at the Sydney Adventist Hospital, Chris O’Brien Lifehouse and he was specifically employed by the Royal Hospital for Women as a specialist breast reconstruction surgeon for the Prince of Wales Campus.
Broadly there are three main types of reconstruction options:
- Implant-based reconstruction – this is either the insertion of implants or tissue expanders to produce a breast mound
- Autologous breast reconstruction – this is using DIEP or muscle-sparing TRAM flaps to use your own tummy tissue to create one or both breasts.
- Autologous and implant reconstruction – this mix and match approach is reserved for patients who have insufficient of their own tissue to create a complete breast reconstruction and also cannot have implants alone due to the risk of complications (such as in radiotherapy). These patients may be suitable for procedures such as latissimus dorsi muscle flap and an implant.
We have taken the time here to note down the most frequently asked questions by our patients regarding breast reconstruction:
Can you sleep on your stomach after breast reconstruction?
This depends on whether own tissue or implants have been used for breast reconstruction.
After a DIEP flap – most of the wounds have healed within 2-3 weeks. It does take around 3 months for flaps to settle with respect to swelling and you are best to wait this time before sleeping on your chest.
After an implant reconstruction – just like any other implants these can move from the pressure of sleeping on your stomach. If these were inserted at the time of mastectomy, you will usually have drains in place. In general, we suggest waiting at least 3 months beyond the time of drain removal before you sleep on your stomach/chest. This is the same recovery times you have to wait before commencing upper body exercise after an implant breast reconstruction.
How long does breast reconstruction take?
The longest breast reconstruction operation is also the best which is the DIEP flap – as they say, no pain, no gain.
The DIEP flap is the Rolls Royce of the Australian society of plastic surgery Breast reconstructions. This is because it uses your own tissue, produces a breast that feels like your own, is permanent that cannot break/rupture/ripple, grows with you with respect to weight gain and weight loss, and also mimics the natural ptosis of breasts with time.
DIEP flap operating time
– For one-sided breast reconstruction with mastectomy – 6-8 hours
– For a bilateral breast reconstruction with mastectomy – 8 to 10 hours
– For one-sided reconstruction without mastectomy – 4-6 hours
– For bilateral breast reconstruction without mastectomy – 6 to 8 hours.
Implant-based breast reconstruction
– Foone-sided breast reconstruction with mastectomy – 2 hours
– For a bilateral breast reconstruction with mastectomy – 4 hours
For one-sided reconstruction without mastectomy:
This will usually involve insertion of breast expanders which takes 1-1.5 hours, but there will be a second stage involving exchange to implants. The length of the second operation depends on if the opposite breast needs surgery in the form of a lift or reduction to match the reconstructed breast. Between the two operations, there are visits to the office to place saline in the expanders to fill the expanders.
For bilateral breast reconstruction without mastectomy – 2 to 3 hours. This will usually involve insertion of breast expanders and there will be a second stage involving exchange to implants which will also take around 2 hours. Between the two operations, there are visits to the office to place saline in the expanders to fill the expanders.
Latissimus dorsi breast reconstruction
– The side of reconstruction takes 4-6 hours with mastectomy and 2-4 hours without mastectomy.

How much is breast reconstruction surgery?
This surgery is offered as a private patient in a private hospital, and as a public patient in the public hospital. For patients without insurance, they can elect to be private patients in a public hospital to reduce their out of pocket costs.
Benefits of a private patient include:
- The convenience of selecting the time of surgery that suits you.
- Direct relationship with breast and plastic surgeon as they manage all your care.
- The procedure is entirely performed by the specialist surgeon of your choosing.
- The follow up is with the surgeon(s) that performed your surgery.
Downsides of a private patient include:
- Mainly the out of pocket cost.
Benefits of a public patient include:
- Cost-free if you are covered by Medicare.
Downsides of a public patient include:
- The inflexibility of time – public hospital lists are by number fewer and booked long in advance with urgent surgeries.
- If you need a mastectomy as well as reconstruction it can be difficult to coordinate the surgeons within the public hospital – and may mean a slight delay.
- Your surgery is performed by training plastic surgeons under the supervision of a specialist plastic surgeon.
- The standard of care is excellent but it is a personal preference if you wish only the senior surgeon to perform the key steps of surgery.
- The inpatient and follow up care is delivered by the registrars and the public hospital.
The Cost:
You will be provided with a quote for a tummy tuck surgery, indicating total and out of pocket expenses, after your consultation. If any complications occur, no further out of pocket costs are incurred, even if this means further surgery. There is no cost associated with breast reconstruction as a public patient in the public hospital. The out of pocket cost of implant-based reconstruction in the private hospital varies, depending on single versus both side reconstruction, and if the opposite breast needs surgery (in the case of single-sided reconstruction).

Is breast reconstruction surgery painful?
In general the larger the surgery the more painful it is – however, we take extensive measures to ensure patients are comfortable and mobile on the first day post surgery.
DIEP flap reconstruction involves surgery on both the breast and the tummy. It is the tummy surgery that slows you down due to the tissue is taken, the long scar and the muscle tightening under the skin. You wake up with your back up, legs bent and need to walk hunched over to protect the scar tissue. We use an extensive amount of local anaesthetic during the surgery, use pain pumps, and the anaesthetist uses excellent pain relief during and after surgery. Most of our patients remark how little pain they had (compared to what they expected) and are out of bed the first postoperative day.
Implant reconstruction, on the other hand, is more straight forward as it only involves the chest – there is no second site that has been operated on, and it does not slow you down like a DIEP flap that involves surgery on the tummy. However patients often expect less pain than they experience as they think this is minor surgery – it is not. The mastectomy alone is uncomfortable and to place implants or expanders at the same time we need to divide a part of the pectoralis major muscle which is painful. We then use a hammock or a sling of tissue called ADM to hold the implant in the correct position – the stitches are placed to the underlying chest wall or ribs and this can also be painful. Again we use a lot of adequate pain relief to make sure you are comfortable postoperatively.
Should I have breast reconstruction after mastectomy?
This is an individual decision but we do recommend that you research it and read up about it. This is because while you may have survived breast cancer and left it in the past it is the aftermath with which you have to face life every day.
Women after mastectomy can be left like completely flat chested:
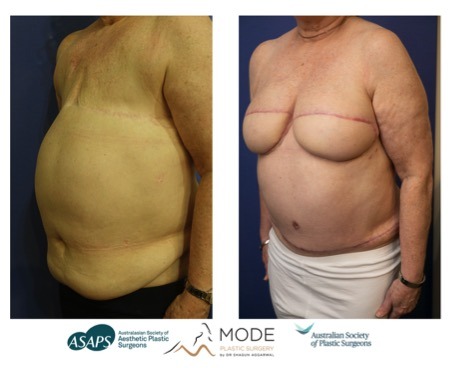
While this may be a cancer-free achievement this person has a constant reminder of the horrible disease she suffered.
Patients, therefore, seek reconstruction to restore their femininity and body image, restore their self-esteem and confidence, feel socially accepted, have some positivity at the end of a cancer journey and minimise stigma.
Breast reconstruction can achieve all these aims and produce an excellent appearance for patients in clothing and often out of clothing as well.
Does medicare cover breast reconstruction?
Yes, Medicare and Health Funds partially cover the cost of breast reconstruction.
There are Medicare item numbers applicable to both own tissue and implant breast reconstruction.
With appropriate health cover, all private hospital fees will be covered by the health funds, and a rebate available for surgeon and anaesthetist fees. This does mean that there is an out of pocket cost associated with being a private patient in a private hospital however this is far less than the actual total cost of surgery, and it would have cost prohibitive without private health insurance to undertake this in a private hospital.
Patients covered by Medicare can also be public patients in a public hospital with no out of pocket costs.
Do you have any further questions? Get in touch!
Email us or call or fill out an enquiry form!

